More Information
Submitted: March 20, 2026 | Accepted: April 17, 2026 | Published: April 20, 2026
Citation: Munawar S, Mahmood F. AI-Driven Hypertension Detection and Risk Prediction: A Comprehensive Review. Ann Clin Hypertens. 2026; 10(1): 001-013. Available from:
https://dx.doi.org/10.29328/journal.ach.1001042.
DOI: 10.29328/journal.ach.1001042
Copyright license: © 2026 Munawar S, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Keywords: Machine learning; Artificial intelligence; Hypertension detection; Risk prediction; Wearable healthcare; ECG; PPG; Healthcare analytics
AI-Driven Hypertension Detection and Risk Prediction: A Comprehensive Review
Sofia Munawar* and Faiza Mahmood
Department of Computer Science, University of Engineering and Technology, Lahore, Pakistan
*Corresponding author: Sofia Munawar, Department of Computer Science, University of Engineering and Technology, Lahore, Pakistan, Email: [email protected]
Hypertension is regarded as one of the most acute global social problems and etiological factors of cardiovascular diseases, stroke, and kidney failure. The early identification and appropriate risk forecasting are the keys to the reduction of morbidity and mortality caused by hypertension. Nevertheless, there have been recent advancements in artificial intelligence (AI) and, particularly, machine learning (ML) and deep learning (DL), which have significantly improved the capacity to detect hypertension and its risk when using various sources of data, such as clinical records, physiological data, and wearable sensor data. The literature review is based on a systematic method of literature selection and the analysis of the latest studies (2020-2025) of large scientific databases. The current review paper provides a general overview of the AI-based hypertension monitoring and prediction methods. It provides a literature review of the field of ML and DL models, datasets, feature engineering techniques, and signal-based monitoring systems. The paper also lists the strengths and weaknesses of the current methods, the problem of the data quality, as well as the interpretability of the model and clinical validation, and multiple future research directions have been specified. Using AI-based solutions is promising immense potential for delivering timely diagnosis, sustained care, and patient-focused care as far as hypertension is concerned.
In this paper, a thorough review of AI-based methods of hypertension detection and risk prediction is presented. It is going to examine the recent developments, compare various machine learning and deep learning models, pinpoint main challenges, and outline the future research directions in the sphere.
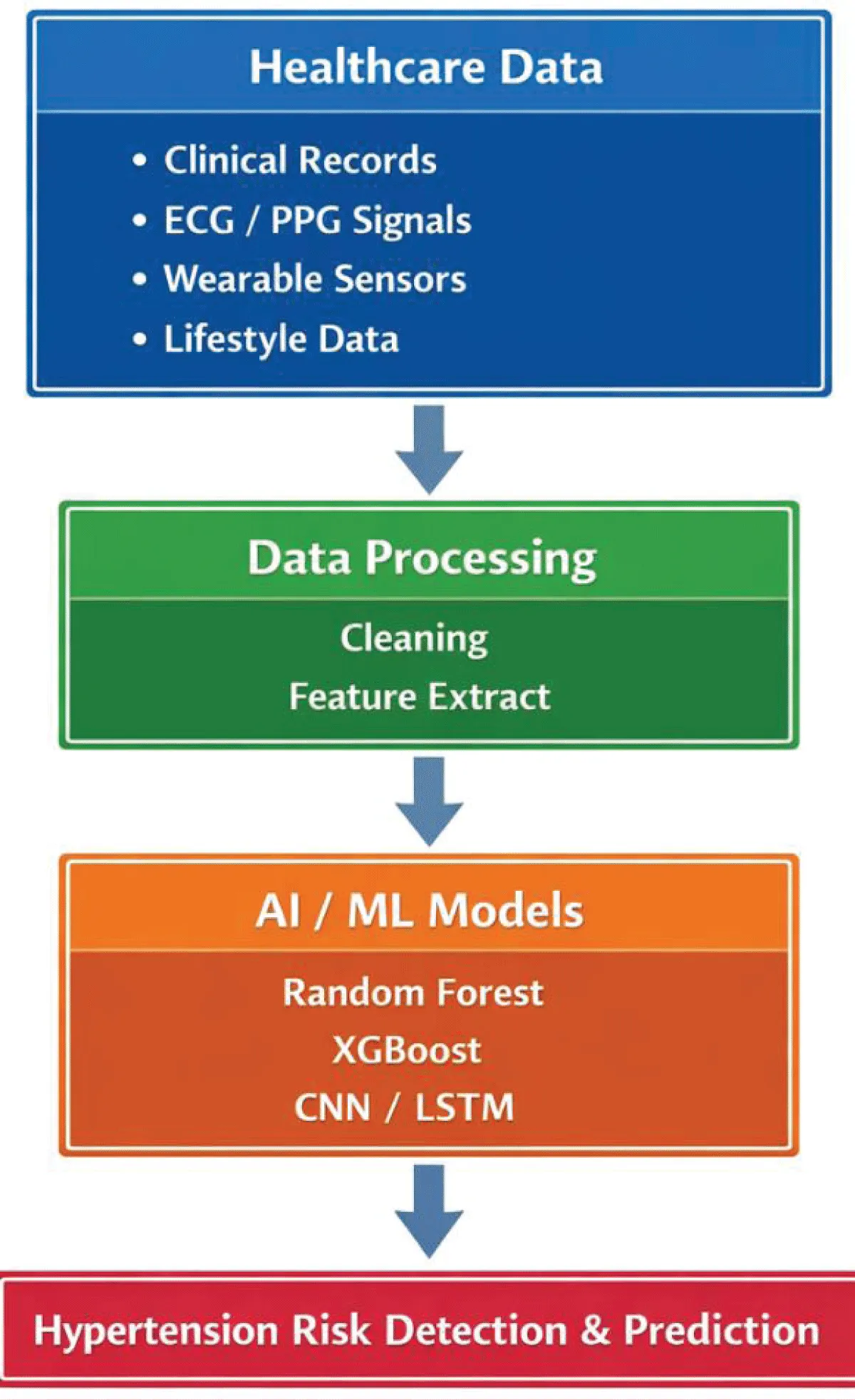
Hypertension is a cardiovascular disease that is very prevalent across the globe. New technologies of Artificial Intelligence (AI) and Machine Learning (ML), have made it possible to predict risks and identify them automatically with the use of clinical data, wearable devices, physiological signals, and wearable devices (Figure 1).
Figure 1: The summary of AI use in the detection of hypertension and risk prediction.
High blood pressure, known as hypertension, stands as a worldwide health problem that significantly raises the probabilities of developing heart conditions and strokes, along with kidney problems. Most people who have hypertension either do not receive diagnosis services or receive limited management services, particularly in low- and middle-income nations [1]. Hypertension develops without symptoms, so people usually discover it only in later dangerous stages when symptoms become apparent. The discovery of early identification methods that offer precise hypertension detection becomes necessary due to this situation. Recent research demonstrates Deep Learning (DL) as a part of Artificial Intelligence (AI), which demonstrates a strong capacity to detect hypertension from its early stages. The analysis capabilities of deep learning models accommodate complex signals from Electrocardiograms (ECG) as well as Photoplethysmograms (PPG) to perform continuous non-invasive blood pressure monitoring [2-4]. The application of these models demonstrates superior speed and accuracy performance when compared to conventional diagnostic methods, according to research presented in [5,6].
Deep learning methods have been extensively examined for hypertension prediction using multiple types of information sources. The NHANES dataset received advanced results when scientists used artificial neural networks from [7]. The research team developed NABNet through a BiConvLSTM architecture, which proved better than traditional methods for continuous blood pressure prediction [8]. BP-Net, together with MML-Net, revealed early cardiovascular signs by analyzing ECG and PPG signals according to research in [3] and [9]. Deep learning, along with machine learning models, demonstrates effectiveness when processing different data, including personal information, medical documents, and lifestyle characteristics. The research study in [10] achieved over 88% accuracy in hypertension predictions through the analysis of 27 features. Researchers trained accurate prediction models by utilizing clinical data, including cholesterol and glucose measurements, in a different study [11]. Large-scale screening demonstrations exist in underserved areas based on these established techniques, according to [12] and [13].
DL-based methods facilitate the creation of wearable technologies for blood pressure monitoring throughout the day without needing cuffs. Two BP detection devices named NeuBP, together with BrainZ-BP, rely on PPG along with brain signals to deliver precise results accompanied by minimal errors, according to research documented in [2] and [14]. These technologies enable health practitioners to identify early indicators of hypertension and customize care as needed, particularly for patients who face high risks of developing hypertension.
Hypertension prediction models absorb two explainable artificial intelligence techniques named SHAP and LIME. Such methods reveal key predictive factors for the systems, which enhance their transparency and trustworthiness for clinical implementations [8]. Further advancement encounters several ongoing obstacles according to research. The effectiveness of DL models heavily relies on obtaining high-quality clinical data, which encompasses diverse information and holds valid medical value because of its approval by doctors and specialists. Research studies both in [15] and [16] highlight the significance of quality data standards alongside structured regulations to enhance healthcare safety when using Artificial Intelligence.
Thus, this research develops a new deep learning system dedicated to early hypertension detection amid existing breakthroughs and obstacles. This method makes use of important health and clinical indicators while incorporating positive aspects from earlier works. The objective of this approach is to improve diagnostic precision while enabling prompt medical action for decreasing the worldwide hypertension prevalence.
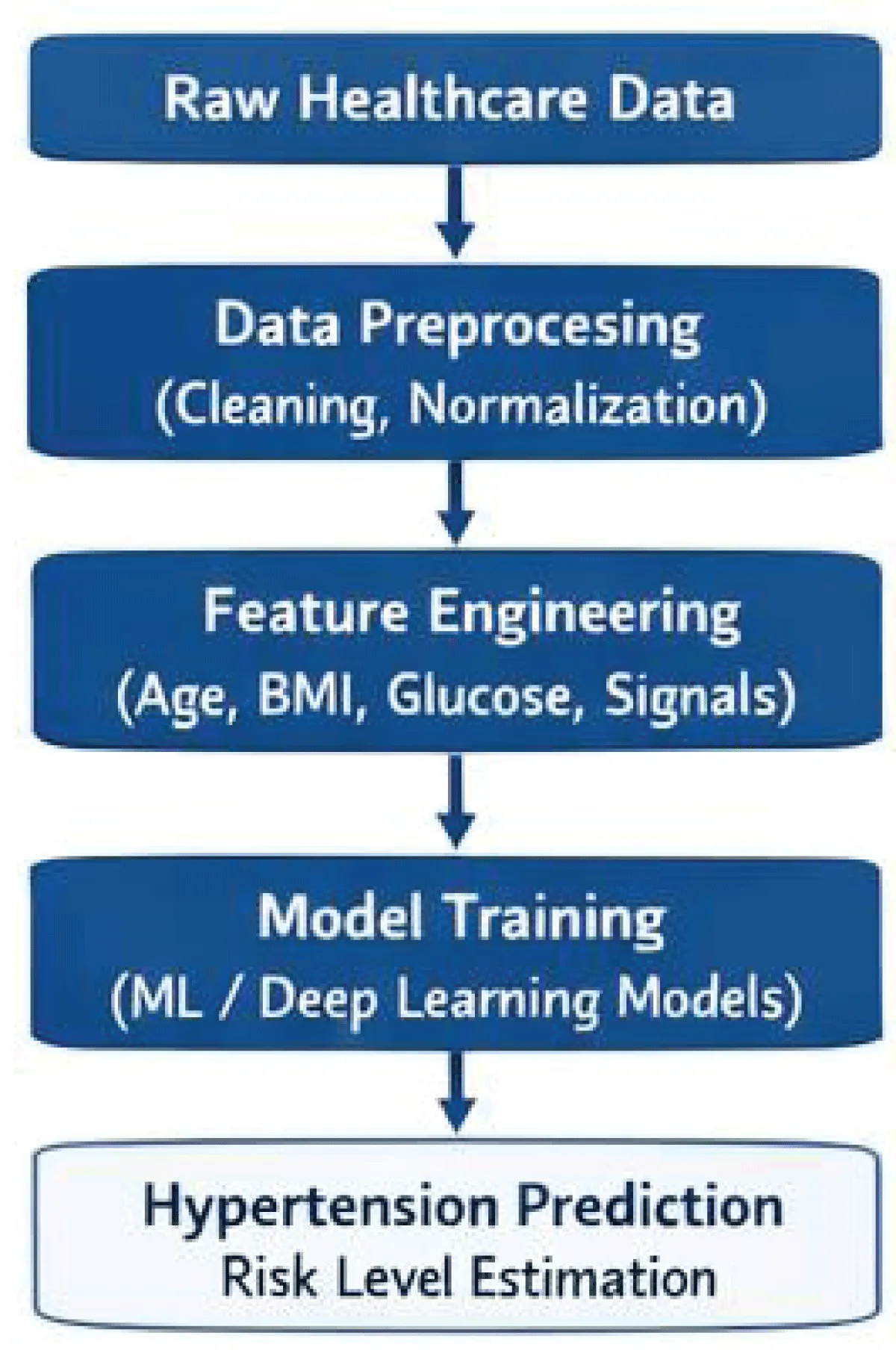
Although there have been tremendous improvements, available literature is usually not standardized, properly validated, and multimodal data is not integrated. Thus, a coherent and contemporary review is needed to comprehend the current trends and research gaps in the prediction of hypertension using AI (Figure 2).
Figure 2: AI framework for hypertension detection and risk prediction using healthcare data and machine learning models.
Fernando López-Martínez, et al. [7] developed a multi-layer Artificial Neural Network (ANN) model to detect early hypertension based on age, BMI, gender, race, kidney disease, diabetes, and smoking factors. They utilized (performed experimentation using) the NHANES dataset that contains the 24,434 records from 2007 to 2016. They achieved performance in terms ofSensitivity: 40%, Specificity: 87%, Precision: 57.8%, Accuracy: 73.2%, and AUC: 0.77, respectively.
Anjan Gudigar, et al. [17] analyzed the potential of different machine learning and deep learning algorithms on physiological signals and imaging modalities based on clinical information. They concluded that the decision tree and random forest achieved the best performance, 99.5% in terms of accuracy.
NCD Risk Factor Collaboration [1] conducted a study focusing on hypertension among 200 different countries with 104 million subjects. Worldwide hypertension rates remain steady between 1990 and 2019 according to their model, while variance in treatment exists among different regions. Control rates received improvements in high-income nations, but low-income nations showed slower progress. Better healthcare, combined with improved policies, needs to reduce hypertension throughout the world, according to the study findings.
Min Fang, et al. [18] employed KNN alongside LightGBM for hypertension risk prediction. The model received training from 23 health and demographic elements extracted from hospital records. A typical accuracy level of 86.06% and an AUC value of 0.9505 were recorded from their approach, which outperformed conventional prediction methods. The authors propose including life habits questions to enhance forecasting accuracy.
NCD Risk Factor Collaboration [19] analyzed 7.5 million people from 181 nations through their hypertension-body fat research. Results indicated that BMI and Waist-to-Height Ratio (WHtR) showed a powerful connection (0.76-0.89) with hypertension. The research findings demonstrated that body mass index does not provide sufficient information to determine hypertension risk. Different obesity measures should be employed when carrying out screening activities according to the study findings.
Hack-Lyoung Kim [20] conducted research to understand the relationship between hypertension and arterial stiffness. The research investigation revealed that elevated PWV parameters, together with endothelial dysfunction and inflammatory conditions, lead to elevated blood pressure levels. PWV and AIx serve as tools suggested by the researcher for early detection of hypertension. Healthcare practices need additional tests to improve their utility.
Manish Sharma et al. [21] examined automatic hypertension detection techniques by analyzing ECG data and supplementary signals, including HRV, PPG, and BCG. The analysis of ECG signals by machine learning yielded 99.99% accuracy, which surpassed results obtained through other signals. The presented research exhibits a need for additional healthcare datasets available to the public. The analysis promotes the development of AI-based wearable tech that monitors blood pressure at all times.
Hygo Sousa De Oliveira, et al. [2] developed NeuBP, which utilizes deep learning algorithms on PPG signals for non-invasive blood pressure measurement of both systolic and diastolic values. NeuBP evaluated on MIMIC-III data delivered systolic blood pressure results with 5.02 mmHg MAE, while diastolic results showed 3.11 mmHg MAE. Researchers demonstrated the ability to use NeuBP technology for monitoring hypertension in wearable devices, yet the system requires a diverse dataset testing for validation purposes.
Chengwei Liang, et al. [3] designed MML-Net as a deep learning model that identifies preliminary heart alterations in ECG signals. The model performed at an 82% recall coupled with 87% precision, which surpassed the ability of cardiologists. Research demonstrates that artificial intelligence offers the capability to identify hypertension during its early stages. Additional testing needs to be performed for various population groups.
Vidhu Anand, et al. [22] developed a detection model of PH through analysis of heart scan record from 7,853 individuals. Gradient boosting enabled their model to reach an AUC score of 0.83, which reflected good accuracy levels. This system functions without depending on specific heart measurement levels. The system demands additional research to become usable in medical practice.
Faezi and Alinezhad [16] conducted research about AI tools used to manage high blood pressure. The researchers established that AI enhances medical care by means of predictive analytics and remote patient monitoring. Programmed intelligence systems together with deep learning technologies produce superior results in hypertension care. The general adoption of AI remains restricted because of data privacy issues and unclear AI model functioning.
Cho and Park [5] conducted research that evaluated AI systems that automate hypertension care through blood pressure assessment and treatment prediction functions. The authors examined smartphone-based and cuff-free AI techniques for BP measurement in their discussion about AI-based BP monitoring systems. The application of machine learning systems effectively detected hypertension, together with forecasting heart risk potential. The practice implementation of AI model validation by nurses becomes necessary because these systems face regulatory constraints as well as privacy issues, along with predetermination biases.
Kaur S, et al. [15] developed a deep learning system that identified hypertension through analysis of Kaggle healthcare information. The investigators used GRU and LSTM along with Bidirectional LSTM, yet Bidirectional GRU showed optimum performance through 99.68% accuracy. An important challenge remained in the study due to data quality requirements and the requirement of clinical verification. The research demonstrates how AI technology identifies heart conditions together with hypertension at their initial phases.
Abdullah & Kristoffersson [23] developed a machine learning method that detects hypertension stages from APG waveforms and medical parameters. Public data served as their database for processing with Decision Trees, together with Linear Discriminant Analysis and Support Vector Machines. Out of the examined models, the Decision Tree achieved the highest accuracy rate at 96.87%. Research demonstrates how APG waveforms serve as a detection tool for hypertension groups, although scientists need to investigate this matter further.
Martinez-Ríos, et al. [24] evaluated machine learning detection methods of hypertension with clinical and physiological information. The authors evaluated multiple models, yet Random Forest delivered the most accurate result. The implementation of the system meets challenges from imperfect data quality combined with deployment complications. Future studies need to focus on resolving existing problems to enhance the capabilities of wearable monitoring systems.
Mohammed Nawi A, et al. [25] researched hypertension experiences among Southeast Asian residents living in cities. The authors reported that 33.82% of participants experienced hypertension because of their age, combined with BMI, smoking, and financial situation. Public health programs, together with lifestyle modifications, were determined to be essential by the study. Research workers demanded specific screening approaches alongside prevention plans for identified high-risk populations.
Shohei Sato [26] examined the assessment of cuffless blood pressure evaluation methods. The researchers combined PPG with ECG to generate a non-contact technique for measurement. The examination of pulse transit time and waveforms served as input for both RNNs and CNNs. The experimental data demonstrated that deep learning technology leads to better blood pressure prediction results.
Massaro, et al. [27] research combined statistics and machine learning to evaluate hypertension risk in 1,007 people. The research used sophisticated models to identify BMI, age, and heart rate as the main determinants. Their methodology proved effective for risk assessment, which enabled predictions of healthcare necessities. Better research outcomes would be possible with additional, larger, and more diverse data sets.
Silva, et al. [28] performed a review of 21 studies regarding machine learning applications for hypertension prediction spanning from 2018 to 2021. The research revealed SVM, Random Forest, and XGBoost as the preferred algorithms because they achieved AUROC scores spanning from 0.766 to 1.00. The authors discussed problems regarding unbalanced data, as well as weak validation methods and insufficient knowledge of handling complex models. The authors proposed the implementation of outcome standards alongside the enhancement of code-sharing methods for better research reproducibility.
Chowdhury, et al. [29] examined 52 research studies that evaluated traditional regression models versus machine learning for hypertension risk assessment. Traditional regression methods produced comparable outcomes according to the study findings. The analysis encountered different issues because researchers used inconsistent mathematical models, performed no external validation, and had restrictions on follow-up information collection. The authors suggest conducting additional validation research and performing studies on actual patient outcomes.
Almansouri, et al. [30] provided a review on how artificial intelligence assists in cardiovascular disease diagnosis, along with identifying early hypertension cases. AI detection systems based on ECG and wearable devices show accurate capabilities to identify heart failure, together with arrhythmias. The analysis presented crucial concerns regarding biased data processing while also showing vulnerabilities to attacks, and it required clinical verification. The paper advocates for AI system implementation in standard medical practice to deliver customized health services.
Mahmud, et al. [31] presented NABNet, which employs BiConvLSTM to generate blood pressure predictions from PPG and ECG waveforms. The results from NABNet as a blood pressure waveform prediction system exceeded traditional methods for ABP evaluation. NABNet provides a potential method to obtain continuous blood pressure readings without invasive techniques. Academic investigations should focus on applying NABNet technology to wearable healthcare systems.
Islam MM, et al. [10] built a hypertension risk screening system through machine learning methods on an Ethiopian data set containing information from 612 participants. The authors selected 27 risk factors through Boruta for feature selection, followed by testing of XGB, RF, ANN, and LR. An XGB model achieved superior performance through 88.81% accuracy, combined with 0.894 AUC measurement. Research data confirmed that age, combined with BMI and diabetes status, together with lifestyle habits, were fundamental risk areas for detecting hypertension early and creating individual treatment plans.
Islam H, et al. [8] analyzed 2,000 blood pressure records to identify abnormalities. The authors employed PCA as well as RFE for feature choice before conducting their assessment of XGBoost, Random Forest, SVM, Decision Tree, and Logistic Regression models. XGBoost model coupled with RFE reached a 91.5% precision rate alongside 0.95 AUC performance values. The XAI methods scored blood pressure changes according to SHAP and LIME analysis, which revealed genetic pedigree along with hemoglobin as pressure-affecting variables.
Du J, et al. [32] developed a hypertension risk prediction system that incorporated data from 1617 individuals. An analysis using MICE and SMOTE, followed by a trial of ten machine learning models, formed the basis of their data preparation work. The best results emerged from LightGBM because it produced 70.57% accuracy while achieving 0.88 AUC. A web system provided quick medical assistance by illustrating how age and ALP, combined with triglycerides and weight, function as predictive risk factors.
Shrivastava, et al. [11] constructed an ML model for blood pressure prediction by analyzing 50,000 clinical data readings. Among the evaluated KNN, Logistic Regression, Decision Tree, and Random Forest algorithms, Random Forest delivered the most successful outcomes. Clinical prediction of blood pressure requires assessing blood sugar levels together with gender information and cholesterol measurements, while also considering smoking behavior, age, and weight status, and the presence of heart disease and alcohol consumption. The model provides an inexpensive system for identifying blood pressure instead of conventional approaches.
Kim H, et al. [6] used deep learning on the KoGES dataset of 8,149 samples for hypertension diagnosis. The network topology consisting of deep neural networks achieved 75% accuracy, which exceeded decision trees (DT). The main contributing factors for hypertension were waist circumference, together with BMI status, diet habits, and sodium consumption. Deep learning enhanced hypertension screening programs by identifying risks during early stages of development for intervention purposes.
Bisong E, et al. [13] applied machine learning techniques to forecast high blood pressure cases within 57 low- and middle-income countries. Within the studied five models, XGBoost proved to deliver the highest accuracy rate at 68.52%. The critical determinants for this analysis consisted of heart rate along with age, weight, and waist measurement. These ML tools demonstrate their ability to assist locations that possess minimal resources, according to the researchers’ analysis.
Nematollahi MA, et al. [33] analyzed body composition and high blood pressure among 4,663 Iranian subjects. Researchers conducted testing of fat, muscle, and metabolism measures to determine their ability to predict hypertension. The AutoMLP model achieved superiority through its 90% accuracy level. The research determined that patient age, together with higher fat levels, raised their hypertension risks, but muscle and metabolic levels decreased their risks.
Yan J, et al. [4] investigated blood pressure prediction through a combination of ECG and PPG and pulse signals examinations. They applied ANN-LSTM to extract valuable features from the signals. The model exhibited high precision through its minimal error rates during the prediction of systolic and diastolic BP values. They demonstrated that multiple input signals enhance the ability to conduct non-invasive blood pressure prediction.
D’Silva, et al. [34] applied machine learning techniques to analyze personal and lifestyle data for hypertension prediction. Evaluation using Random Forest, as well as Decision Tree and Logistic Regression, achieved an accuracy rate of approximately 82%. A total of seven variables, including age, gender, education level, job type, smoking behavior, exercise habits, diet quality, and family background history, proved significant according to the study. The research investigation established machine learning as a method to detect hypertension risks in the early stages.
Wang, et al. [35] applied deep learning algorithms to MRI imagery for detecting between HCM and HHD cardiac conditions. The trained ResNet32 model produced superior performance to previous methods. The model achieved a satisfactory AUC score, reaching 0.830. Deep learning technology demonstrates its value as a tool for medical professionals to detect heart diseases more effectively.
Islam, et al. [12] analyzed hypertension prediction through machine learning with information collected from Bangladesh, Nepal, and India. This research team analyzed data from 818,603 participants to test XGBoost, GBM, LDA, Decision Tree, Random Forest, and Logistic Regression models. XGBoost, together with GBM and LDA, achieved 90% accuracy by using BMI and age as essential risk factors. The research demonstrates how ML technology enables mass hypertension assessments that benefit public health programs.
Montagna S, et al. [36] established a hypertension detection framework using machine learning that processed information from around 20,000 Italian participants. Undersampling of data with the Random Forest model produced the most effective results by discovering 81.8% of cases with an AUC score of 0.816. A study showed that machine learning models demonstrated better sensitivity than medical protocols, although they required improvement to achieve practical healthcare uses. The research demonstrates potential applications for ML in healthcare, although it acknowledges the necessity for more development.
Dubey AK, et al. [37] developed a heart disease classification system using deep learning with the Crow Search Optimization Algorithm (CSOA) for feature selection. They analyzed two datasets: Cardio (70,000 instances) and NIH Chest X-ray (122,120 images). The CSOA-DNN model with the Nadam optimizer achieved 96.5% accuracy. This study shows CSOA’s effectiveness in both classification accuracy and dimensionality reduction.
Estiko RI, et al. [38] analyzed 38 research papers that evaluated the usage of machine learning to predict hypertension based on basic risk factors, including age, gender, BMI, smoking, physical activity, and diet. Random Forest algorithms yielded outstanding performance with an AUC of 0.92 when predicting hypertension statuses according to their findings. The research demonstrates the key importance of machine learning methods in identifying hypertension at an early stage. The early detection of hypertension risks can occur through population screening, which starts interventions at the right time.
Wang R, et al. [39] established the Physics-Informed Temporal Network (PITN), which measures blood pressure without cuffs through the combination of bioimpedance and PPG and millimeter-wave sensors. The model implements adversarial training together with contrastive learning to enhance its accuracy performance. PITN established 31% superior correlation while delivering RMSE values that were 14% lower compared to traditional model procedures. AI enables the integration of blood pressure measurement technology into wearable medical systems, according to the findings of this study.
Tang Q, et al. [40] established the Data-Knowledge Co-Driven Feature DKCF model for blood pressure level predictions from PPG signals. Better accuracy results from combining both data features alongside knowledge-based features in the model. The model achieved the minimum values in MAE and RMSE measurements for systolic and diastolic BP assessments with two subject groups. The addition of physiological understanding enhances the hypertension diagnosis capabilities of ML-based assessment methods, according to this study.
Yang B, et al. [14] developed BrainZ-BP, a catheter-free system for blood pressure measurement through ECG and brain bioimpedance data analysis. A total of 13 test subjects participated in the system, which generated measurement errors of 2.17 mmHg in SBP and 1.71 mmHg in DBP. The system achieved a high correlation of 0.90 when measuring SBP values. Further studies involving extensive datasets must verify the system’s capability to monitor intracranial pressure and blood pressure correctly.
Turnip A, et al. [41] developed a Support Vector Regression (SVR) system that used PPG signals to forecast blood pressure levels. A total of 110 participants underwent testing in the dataset that contained heart rate and interbeat interval readings. Evaluation showed high prediction accuracy, amounting to 94.06% for systolic BP and 91.18% for diastolic BP. This research concludes that SVR-based blood pressure estimation delivers effective results through wearable healthcare devices.
Elahi A, et al. [42] investigated hypertension rates across Pakistan and discovered 46.2% of people suffer from the condition, yet treatment success rates remain low. The main obstacles stem from patients disregarding their medicine guidelines and insufficient medical insurance coverage, together with inadequate doctor-patient communication. The research indicates that Pakistan requires reasonably priced healthcare as well as digital management solutions to address hypertension effectively. The research needs to expand its focus on the population to establish methods of controlling the growing case numbers.
Ankışhan H, et al. [43] created a speech-based prediction system for blood pressure measurements through the implementation of Graph Diffusion Network (GDN). A total of 127 people provided speech data, which served as the basis for training through Mel-Frequency Cepstral Coefficients (MFCCs). The GDN model exhibited exceptional accuracy because systolic BP demonstrated an R² of 0.965, alongside diastolic BP showing an R² of 0.935. The results demonstrate that speech analysis technology can become an effective tool for both quick and continuous blood pressure evaluation.
Hasanzadeh N, et al. [44] analyzed PPG signals through random convolution methods to identify hypertension instances. Their model received training from 3750 subject databases, then applied testing on 625 additional participants. When using Random Forest as its classification algorithm, MiniROCKET delivered the highest F1-score at 71.6%. The research evidence reveals how wearable technology supports the identification of high blood pressure at an early stage.
Islam SMS, et al. [45] employed machine learning techniques to forecast hypertension susceptibility levels among people from Bangladesh, Nepal, and India. A large health survey database received tests from the researchers who compared Decision Tree against Random Forest, as well as XGBoost and Logistic Regression. Using GBM models on XGBoost produced the peak results with 90% accuracy and complete recall through age and BMI variables. This research indicates ML technology supports extensive screening operations even though it requires better medical information.
Baharoon M, et al. [46] created HyMNet, which functions as a deep learning system to identify hypertension. The study incorporated five thousand sixteen eye images from one thousand two hundred and forty-three participants while utilizing health and demographic data. The team achieved favorable performance metrics from their best model, IntermediateFusion, which reached an F1-score level of 0.771. The research demonstrates that AI processing of eye images contributes to hypertension diagnosis, yet expanded datasets will enhance its effectiveness.
Duffy G, et al. [47] introduced EchoNet-LVH, which serves as a tool for deep learning detection of heart muscle thickening through echo videos. The tool underwent testing on more than 24,000 videos at the same time, and researchers validated results with additional hospital videos. Experimental results indicated that the model performed well in heart size assessment while detecting heart diseases efficiently. The research demonstrates that artificial intelligence technology assists with heart screening, yet additional examinations should focus on various scan protocols.
Vardhan KR, et al. [9] developed BP-Net as a deep learning model for BP measurement using continuous PPG signals. The U-Net architecture in BP-Net processed MIMIC-II Waveform Database data to achieve 5.16 mmHg SBP MAE and 2.89 mmHg DBP MAE. The system demonstrated its feasibility for real-time edge inference on Raspberry Pi when deployed for wearable blood pressure monitoring solutions.
Evdochim L, et al. [48] developed the ML-based ANC Test™ system, which detects hypertension through processing PPG signals. The research team analyzed data from China and MIMIC-III for distinguishing between individuals who had or did not have high blood pressure. The best model, identified as Quadratic SVM, achieved a 72.9% accuracy rate. Better integration of datasets is presented as one major challenge, for which they proposed new improvements in ML model creation.
Mroz T, et al. [49] utilized ML to forecast hypertension control in 12 months based on 350,008 Cleveland Clinic EMR patients. Using 793 training variables, the XGBoost model produced results that showed a measurement of 0.756 AUC and identified medication adherence levels together with systolic BP trends as major predictive factors. The study indicates ML shows promise in optimizing hypertension treatment, although external verification must be performed to extend its practical value.
Madhumitha S, et al. [50] applied ML models to predict hypertension status based on Kaggle dataset information from systolic and diastolic BP measurements. The LightGBM model achieved the best performance with a 92% accuracy compared to CatBoost, XGBoost, and Random Forest solutions. ML-based screening of hypertension remains significant, but researchers need to study additional factors such as genetics and life habits to improve prediction accuracy.
Effati S, et al. [51] created a web-based machine learning system that predicts heart disease and hypertension risks in miners. Fabia, Nils, Walther, and Ajami examined 699 Iranian miners through combinations of occupational, health, and personal information. Random Forest, together with XGBoost, achieved predictions for hypertension with 99% accuracy, while they predicted heart disease with 97% accuracy. The research demonstrates work environment effects on health status while demonstrating the benefits of ML for early diagnosis.
Literature overview
Recent studies have delved into several artificial intelligence methods used to identify cases of hypertension, as well as forecast cardiovascular risk. Such studies are based on the various forms of data, such as clinical features, physiological signals, imaging, and lifestyle data. Among the possible solutions that were offered at the very beginning was the one by Lopez-Martinez, et al. [7], where the authors created a multilayer artificial neural network based on such demographic and clinical factors as age, gender, BMI, smoking habits, and the presence of diabetes. The model was trained on the NHANES data that had 24,434 records, and the model had an accuracy of 73.2% and an AUC of 0.77. This paper revealed the possibility of neural networks for detecting people at risk of hypertension.
More recent research has delved into the hybrid machine learning models to enhance the accuracy of prediction. In the article by Fang, et al. [18], K-Nearest Neighbors (KNN) was applied along with LightGBM based on electronic health records with demographical and clinical variables. Their model had an accuracy of 86.06 and an AUC of 0.9505, showing the significance of using a combination of feature engineering and sophisticated machine learning methods. The interaction between physiological indicators and hypertension has also been explored by a number of researchers. Kim [20] evaluated the posture of the arteries and established the Pulse Wave Velocity (PWV) and Augmentation Index (AIx) as some of the cardinal clues linked to high blood pressure. Depending on them in AI prediction models, it can enhance early detection of these physiological measurements.
Non-invasive hypertension detection has also received much attention in physiological signal analysis. Sharma, et al. [21] evaluated ECG, HRV, PPG, and ballistocardiography signals with the help of machine learning algorithms. Their results revealed that ECG-based models had incredibly high levels of accuracy, which reached 99.99. These findings show that signal-based analysis could be used in real-time to detect hypertension. The analysis of the physiological signals has also been improved through deep learning methods. As an example, Oliveira, et al. [2] presented NeuBP, a depth neural network that approximates systolic and diastolic blood pressure based on PPG data of the MIMIC-III database. The model obtained an average error of 5.02 mmHg and 3.11 mmHg in systolic and diastolic pressure respectively.
On the same note, Liang, et al. [3] came up with MML-Net, a deep learning model that seeks to identify emergent cardiovascular alterations with hypertension through the analysis of ECG signals. The model had a precision of 87 percent and a recall of 82 percent, which are similar to those of the experienced cardiologists. Multimodal data analysis is also another approach that has potential and offers greater predictive outcomes by integrating multiple data types. Baharoon, et al. [46] created a deep learning framework named HyMNet, which integrates retinal fundus imagery as well as clinical characteristics to identify hypertension. Our system was able to get an F1-score of 0.771, showing that the use of visual biomarkers can be used to help diagnose hypertension.
There have also been population-level studies that have been informative on the factors of risk of hypertension. As an example, Islam, et al. [12] evaluated the data of a demographic health survey in Bangladesh, Nepal, and India with the help of various machine learning algorithms. Their findings revealed that models like XGBoost and Gradient Boosting performed about 90 percent in risk prediction of hypertension. Wearable technologies are also being applied in continuous blood pressure monitoring in addition to clinical datasets. Deep learning frameworks, including BP-Net and NABNet, are used to predict the blood pressure based on PPG and ECG signals. Cuff-less blood pressure monitoring and continuous monitoring are possible in such systems; the systems are applicable in real-time healthcare. In general, according to the literature, machine learning and deep learning models can substantially enhance the process of predicting and detecting hypertension. Their performance, however, differs when used in relation to the quality of the dataset used, the methods used in feature selection, and the model architecture.
The review is organized in terms of searching and evaluating pertinent literature about the AI-based hypertension detection and prediction.
Major scientific databases such as Google Scholar, PubMed, IEEE Xplore, and ScienceDirect were searched to find the relevant studies.
The main search terms were: Hypertension Prediction, Artificial Intelligence in Healthcare, Machine Learning, Deep Learning, ECG, and PPG-based hypertension detection.
Inclusion criteria involved:
- Articles that were published in 2020-2025.
- Articles written in English.
- Studies in the field of AI/ML/DL in the detection of hypertension.
Exclusion criteria included:
- Studies with incomplete results.
- Non-peer-reviewed articles.
- Irrelevant or duplicate studies.
The analysis of a total of selected papers was performed in terms of methodology, dataset, performance metrics, and limitations.
Analytical review of AI-based hypertension detection
The vast body of literature on artificial intelligence applications in hypertension detection also indicates that there is a big step forward in predictive healthcare analytics. The analyzed literature demonstrates that machine learning and deep learning algorithms are suitable to determine the risk of hypertension based on many forms of biomedical evidence, such as clinical records, physiological measurements, radiography, and lifestyle factors. To learn how research based on AI investigation of the hypertension topic has evolved, the results may be grouped into several key analytic themes (Figure 3).
Figure 3: General workflow of AI-based hypertension prediction systems.
Data sources used to predict hypertension
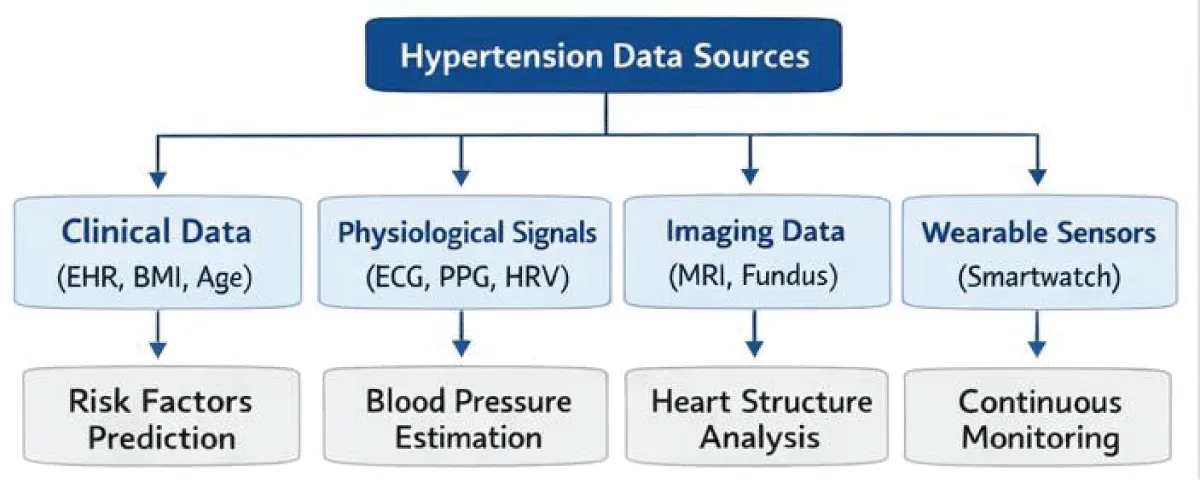
AI models detecting hypertension have been applied to different types of datasets. These data sets can be essentially divided into four groups (Figure 4).
Figure 4: Major data sources used for AI-based hypertension prediction.
1. Clinical and demographic data
Clinical datasets contain one’s data, such as age, BMI, cholesterol level, blood glucose, smoking, and family medical history. Most of the studies are based on such structured datasets, as they are readily available in Electronic Health Records (EHRs).
Key findings include:
- Lopez-Martinez, et al. [7] used the NHANES data containing over 24,000 records and managed to get a score of 73.2% accuracy using the neural networks.
- Fang, et al. [18] used KNN and LightGBM to get an AUC of 0.95, which proves the usefulness of hybrid models.
- Islam, et al. [10]returned on 27 clinical features and had an 88.81 accuracy with XGBoost.
These papers suggest that structured clinical features are one of the most accurate predictors of hypertension risk.
2. Physiological signals
ECG, PPG, HRV, and BCG are examples of physiological signals that give real-time data on the activity of the cardiovascular system.
Important observations include:
- Sharma et al. [21] had 99.99% accuracy with ECG-based machine learning models.
- NeuBP used PPG signals and had small errors of prediction, 5.02 mmHg (SBP) and 3.11 mmHg (DBP).
- BP-Net and NABNet implemented deep learning models to provide a good estimation of blood pressure at continuous time.
These results show that signal-based AI models can be used to develop non-invasive monitoring systems.
3. Medical imaging data
Medical imaging has been investigated in recent studies to detect hypertension.
Examples include:
- HyMNet was used to predict retinal fundus images with clinical information to attain an F1-score of 0.771.
- ResNet32 MRI-based deep learning models also performed well on the detection of abnormalities related to the heart that are related to hypertension.
Such multimodal handicrafts will enable AI systems to examine structural variations in organs in reference to hypertension.
4. Wearable and sensor data
The wearable technology offers constant recording of physiological cues and lifestyle.
Significant advances it has made are:- Cuff-less blood pressure, BrainZ-BP, and PITN.
- Wearable PPG-based cardiovascular monitoring systems.
- Smart devices that are integrated with AI allow remote monitoring of patients.
Wearable technologies are a good avenue towards real-time monitoring of hypertension.
Used machine learning algorithms
There are various machine learning algorithms that have been popular in the prediction of hypertension (Figure 5).
Figure 5: Machine learning and deep learning models are commonly used in hypertension detection systems.
Conventional machine learning models
In the most common use, algorithms are:
- Logistic Regression
- Decision Trees
- Random Forest
- Support Vector Machines
- Gradient Boosting
- XGBoost
Random Forest and XGBoost are often better than the other traditional algorithms since they are capable of dealing with nonlinear correlation and complex interactions between features.
Deep learning models
The capability to handle high-dimensional data has made deep learning methods more popular.
There is a wide use of architectures such as:
- Convolutional Neural Networks (CNN)
- Long Short-Term Memory networks (LSTM)
- Bidirectional GRU
- Hybrid CNN-LSTM models
- BiConvLSTM architectures
The models are especially effective with time-series biomedical signals like ECG and PPG.
Importance of the features in the prediction of hypertension
Some of the studies presented significant predictors of hypertension risk.
Most prevalent risk factors may comprise:
- Age
- Body Mass Index (BMI)
- Waist-to-Height Ratio
- Blood glucose levels
- Cholesterol levels
- Smoking habits
- Physical activity
- Sodium intake
- Hypertension in the family history
Nematollahi, et al. [33] and Islam, et al. [8] studies revealed that clinical indicators in combination with lifestyle factors are very effective in prediction.
Explainable Artificial Intelligence (XAI)
Model interpretability is one of the greatest problems of AI healthcare systems.
To escape this problem, explainable AI techniques have been included in a number of studies.
Common XAI techniques:
- SHapley Additive Explanations SHAP
- LIME Local Interpretable Model-Agnostic Explanations LIME.
This is achieved by the techniques that determine the contribution of each feature used in the prediction process.
For example:
- Islam, et al. applied SHAP analysis to establish the level of hemoglobin and the impact of genes on blood pressure.
- Several studies explained predictions made by deep learning models using LIME.
Explainable AI enhances faith, unexploredness, and clinical utilization of AI frameworks.
Comparative performance analysis
According to the literature, the performance of the models can be different based on the type of data set and the methods of selecting features.
The general observations include:
- Signal-based deep learning models are usually the most accurate.
- The hybrid ML models are more effective than single algorithms.
- Big data of the population enhances the generalizability of the models.
Nevertheless, other studies have very high accuracy (more than 99%), possibly due to overfitting or bias in the data.
As such, extrinsic validation and cross-dataset assessment are critical.
Trends and future directions of research
The review of the recent publications shows that there are various emerging trends.
1. Multimodal learning
The use of both clinical records, imaging, and physiological signals as a combination of multiple data sources enhances the performance of prediction.
2. Wearable monitoring and AI on edges
More and more AI models are being implemented on wearable devices to monitor health in real-time.
3. Personalized medicine
There can be AI systems that facilitate individual risk-based treatment plans.
4. Population-scale screening
Machine learning algorithms could be applied to huge healthcare datasets to detect populations at risk.
Critical research gaps
There are still a number of research gaps, even with the great advancement made.
Data Challenges
- There is a scarcity of big annotated databases.
- Ineffective medical datasets.
- Absence of standardized data forms
Model challenges
- Deep learning models are not explainable.
- Risk of overfitting
- Weak cross-population confirmation.
Problematic issues in clinical implementation
- Data privacy concerns
- Regulatory approval issues.
- Connections with health care systems.
The challenges must be overcome to translate AI-based models of hypertension prediction into clinical practice.
The analyzed literature shows that there are several significant trends in hypertension detection with the use of AI. To begin with, machine learning algorithms like Random Forest, XGBoost, and Gradient Boosting have shown high performance when they are used on structured clinical data. The models have been especially successful in use with feature selection algorithms, including recursive feature elimination and Boruta. Second, deep learning-based methods have demonstrated excellent performance in the analysis of physiological signals and medical imaging data. CNNs, LSTMs, and hybrid architectures are the models that can be used to identify temporal changes in ECG and PPG signals and predict blood pressure fluctuations correctly. Third, when wearable technology is combined with AI, they have made it possible to constantly monitor blood pressure without invasive procedures. These systems can revolutionize healthcare since they can be detected in real time, and early intervention against hypertension can be made. Although these advancements have been made, there are a number of limitations. Most research uses relatively small datasets, and this can have a limited generalization of their models. Moreover, the fact that data preprocessing and evaluation metrics vary across studies makes it challenging to explicitly compare the outcomes of studies.
Challenges and Limitations
Even though AI-based systems of hypertension detection demonstrate promising outcomes, there are a number of challenges that would have to be overcome before they can be widely used in clinical practices. Access to quality datasets is one of the most significant challenges. Most of the current datasets have missing data, unbalanced classes, or even lack diversity in population, which may adversely affect the performance of a model. Model interpretability is also another critical consideration. Deep learning models are typically black boxes, and hence, clinicians cannot easily comprehend how the model arrives at predictions. Explainable AI methods, including SHAP and LIME, have been suggested as solutions to this issue, although additional work is required. Privacy and security of data are also important issues, particularly when it comes to sensitive healthcare information. To achieve credible AI systems, it is necessary to ensure that people adhere to the data protection regulations. Lastly, numerous AI models are not externally clinically verified. It is hard to evaluate them in the real-life context of healthcare without mass testing.
Future research directions
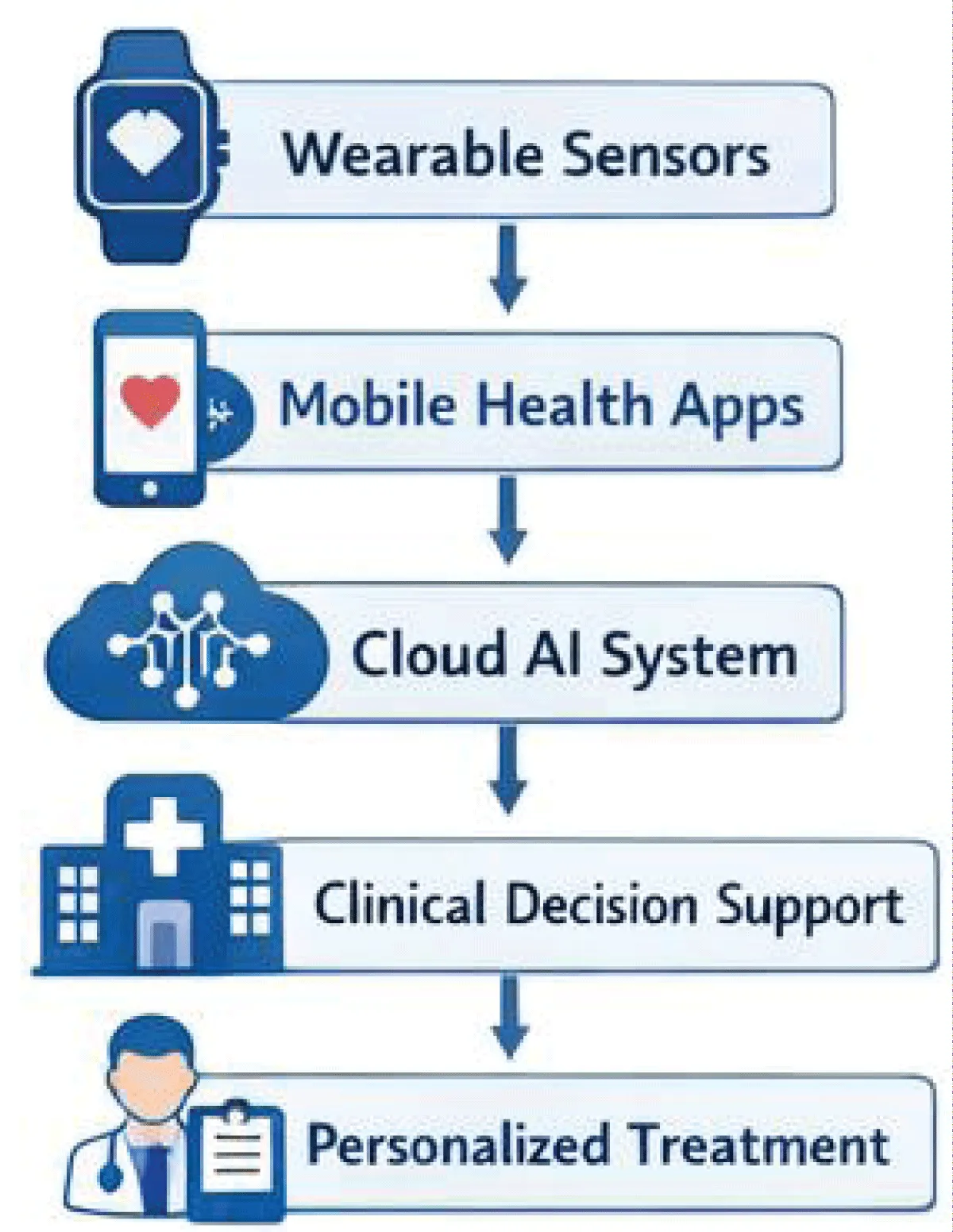
The research on AI-based hypertension detection in the future should address some key areas. First, the creation of large and diverse publicly accessible datasets will enhance model reliability and enable us to compare algorithms better. Second, the researchers are encouraged to pursue multimodal learning methods that integrate clinical information, physiological information, and imaging information. These kinds of models can be able to capture complicated relations among various health indicators. Third, enhancing the interpretability of the model will be important in securing the confidence of health practitioners. Predictive models with explainable AI applications can also enable clinicians to gain a clearer insight into and confirm AI-made predictions. Lastly, AI will be useful in the future of hypertension monitoring when combined with wearable healthcare devices. The monitoring systems could be continuous and would raise warning signals and facilitate individualized treatment plans (Figure 6).
Figure 6: Future AI-enabled ecosystem for real-time hypertension monitoring and personalized healthcare.
Artificial intelligence has become one of the potent tools for enhancing hypertension detection and risk prediction. The machine learning and deep learning models can process huge and complex healthcare data and find patterns that cannot be observed through conventional statistical methods. The technologies allow the early identification, constant observation, and individual health care management of individuals at risk of hypertension. The reviewed papers in this paper indicate that AI-based models can attain high accuracy rates when used in clinical data, physiological signal data, and medical imaging data. Nonetheless, there are still a number of challenges, such as data quality, interpretability of the model, and the large-scale clinical validation requirement. These issues will be critical in the process of transferring AI-based hypertension-detecting systems in laboratory settings to actual healthcare settings. As ongoing innovations in data science and healthcare technology, AI can profoundly enhance the management of hypertension and minimize the volume of cardiovascular diseases in the world.
- NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in hypertension prevalence and progress in treatment and control from 1990 to 2019: a pooled analysis of 1201 population-representative studies with 104 million participants. Lancet. 2021 Sep 11;398(10304):957-980. Available from: https://doi.org/10.1016/s0140-6736(21)01330-1
- De Oliveira HS, Pinto RA, Souto EJP, Giusti R. Estimation of systolic and diastolic blood pressure for hypertension identification from photoplethysmography signals. Appl Sci. 2024;14(6):2470. Available from: https://www.mdpi.com/2076-3417/14/6/2470
- Liang C, Yang F, Huang X, Zhang L, Wang Y. Deep learning assists early detection of hypertension-mediated heart change on ECG signals. Hypertens Res. 2025;48:681-692. Available from: https://doi.org/10.1038/s41440-024-01938-7
- Yan J, Wang Z, Guo R, Yan H, Wang Y, Qiu W. Blood pressure prediction based on multi-sensor information fusion of electrocardiogram, photoplethysmography, and pressure pulse waveform. Measurement. 2025;240:115446. Available from: https://ui.adsabs.harvard.edu/abs/2025Meas..24015446Y/abstract
- Cho JS, Park JH. Application of artificial intelligence in hypertension. Clin Hypertens. 2024;30(1):11. Available from: https://doi.org/10.1186/s40885-024-00266-9
- Kim H, Hwang S, Lee S, Kim Y. Classification and prediction on hypertension with blood pressure determinants in a deep learning algorithm. Int J Environ Res Public Health. 2022;19(22):15301. Available from: https://doi.org/10.3390/ijerph192215301
- López-Martínez F, Núñez-Valdez ER, Crespo RG, García-Díaz V. An artificial neural network approach for predicting hypertension using NHANES data. Sci Rep. 2020 Jun 30;10(1):10620. Available from: https://doi.org/10.1038/s41598-020-67640-z
- Islam H, Iqbal MS, Hossain MM. Blood pressure abnormality detection and interpretation utilizing explainable artificial intelligence. Intell Med. 2025;5(1):54-65. Available from: https://doi.org/10.1016/j.imed.2024.09.005
- Vardhan KR, Vedanth S, Poojah G, Abhishek K, Kumar MN, Vijayaraghavan V. BP-Net: efficient deep learning for continuous arterial blood pressure estimation using photoplethysmogram. In: 2021 IEEE Int Conf Mach Learn Appl (ICMLA); 2021. p. 1495-1500. Available from: https://doi.org/10.48550/arXiv.2111.14558
- Islam MM, Alam MJ, Maniruzzaman M, Ahmed NAMF, Ali MS, Rahman MJ, et al. Predicting the risk of hypertension using machine learning algorithms: a cross-sectional study in Ethiopia. PLoS One. 2023 Aug 24;18(8):e0289613. Available from: https://doi.org/10.1371/journal.pone.0289613
- Shrivastava A, Chakkaravarthy M, Shah MA. A new machine learning method for predicting systolic and diastolic blood pressure using clinical characteristics. Healthc Anal. 2023;4:100219. Available from: https://doi.org/10.1016/j.health.2023.100219
- Islam SMS, Talukder A, Awal MA, Siddiqui MMU, Ahamad MM, Ahammed B, et al. Machine learning approaches for predicting hypertension and its associated factors using population-level data from three South Asian countries. Front Cardiovasc Med. 2022;9:839379. Available from: https://doi.org/10.3389/fcvm.2022.839379
- Bisong E, Jibril N, Premnath P, Buligwa E, Oboh G, Chukwuma A. Predicting high blood pressure using machine learning models in low- and middle-income countries. BMC Med Inform Decis Mak. 2024;24(1):234. Available from: https://doi.org/10.1186/s12911-024-02634-9
- Yang B, Liu L, Wu W, Zhou M, Liu H, Ning X. BrainZ-BP: a noninvasive cuff-less blood pressure estimation approach leveraging brain bio-impedance and electrocardiogram. IEEE Trans Instrum Meas. 2023;73:1-13. Available from: https://doi.org/10.48550/arXiv.2311.10996
- Kaur S, Bansal K, Kumar Y, Changela A. A comprehensive analysis of hypertension disease risk factors, diagnostics, and detections using deep learning-based approaches. Arch Comput Methods Eng. 2024;31(4):1939-1958. Available from: https://doi.org/10.1007/s11831-023-10035-w
- Faezi A, Alinezhad B. AI-enhanced health tools for revolutionizing hypertension management and blood pressure control. InfoScience Trends. 2024;1(1):67-72. Available from: https://doi.org/10.61186/ist.202401.01.08
- Gudigar A, Kadri NA, Raghavendra U, Samanth J, Maithri M, Inamdar MA, et al. Automatic identification of hypertension and assessment of its secondary effects using artificial intelligence: A systematic review (2013-2023). Comput Biol Med. 2024 Apr;172:108207. Available from: https://doi.org/10.1016/j.compbiomed.2024.108207
- Fang M, Chen Y, Xue R, Wang H, Chakraborty N, Su T, et al. A hybrid machine learning approach for hypertension risk prediction. Neural Comput Appl. 2023;35(20):14487-14497. Available from: https://doi.org/10.1007/s00521-021-06060-0
- NCD Risk Factor Collaboration (NCD-RisC). General and abdominal adiposity and hypertension in eight world regions: a pooled analysis of 837 population-based studies with 7.5 million participants. Lancet. 2024 Aug 31;404(10455):851-863. Available from: https://doi.org/10.1016/s0140-6736(24)01405-3
- Kim HL. Arterial stiffness and hypertension. Clin Hypertens. 2023;29:31. Available from: https://doi.org/10.1186/s40885-023-00258-1
- Sharma M, Rajput JS, Tan RS, Acharya UR. Automated detection of hypertension using physiological signals: A review. Int J Environ Res Public Health. 2021;18(11):5838. Available from: https://doi.org/10.3390/ijerph18115838
- Anand V, Weston AD, Scott CG, Kane GC, Pellikka PA, Carter RE. Machine learning for diagnosis of pulmonary hypertension by echocardiography. Mayo Clin Proc. 2024;99(2):260-270. Available from: https://doi.org/10.1016/j.mayocp.2023.05.006
- Abdullah S, Kristoffersson A. Machine learning approaches for cardiovascular hypertension stage estimation using photoplethysmography and clinical features. Front Cardiovasc Med. 2023;10:1285066. Available from: https://doi.org/10.3389/fcvm.2023.1285066
- Martinez-Ríos E, Montesinos L, Alfaro-Ponce M, Pecchia L. A review of machine learning in hypertension detection and blood pressure estimation based on clinical and physiological data. Biomed Signal Process Control. 2021;68:102813. Available from: https://doi.org/10.1016/j.bspc.2021.102813
- Mohammed Nawi A, Mohammad Z, Jetly K, Abd Razak MA, Ramli NS, Wan Ibadullah WAH, et al. The prevalence and risk factors of hypertension among the urban population in Southeast Asian countries: a systematic review and meta-analysis. Int J Hypertens. 2021;2021:6657003. Available from: https://doi.org/10.1155/2021/6657003
- Sato S. Method for blood pressure estimation. Scispace. 2021.
- Massaro A, Giardinelli V, Cosoli G, Magaletti N, Leogrande A. Hypertension risk prediction. J Predict Anal. 2022. Available from: https://doi.org/10.21203/rs.3.rs-1708299/v1
- Silva GF, Fagundes TP, Teixeira BC, Chiavegatto Filho AD. Machine learning for hypertension prediction: a systematic review. Curr Hypertens Rep. 2022;24(11):523-533. Available from: https://doi.org/10.1007/s11906-022-01212-6
- Chowdhury MZI, Naeem I, Quan H, Leung AA, Sikdar KC, O’Beirne M, et al. Prediction of hypertension using traditional regression and machine learning models: a systematic review and meta-analysis. PLoS One. 2022;17(4):e0266334. Available from: https://doi.org/10.1371/journal.pone.0266334
- Almansouri NE, Awe M, Rajavelu S, Jahnavi K, Shastry R, Hasan A, et al. Early diagnosis of cardiovascular diseases in the era of artificial intelligence: an in-depth review. Cureus. 2024;16(3):e55869. Available from: https://doi.org/10.7759/cureus.55869
- Mahmud S, Ibtehaz N, Khandakar A, Rahman MS, Gonzales AJ, Rahman T, et al. NABNet: a nested attention-guided BiConvLSTM network for robust prediction of blood pressure components from reconstructed arterial blood pressure waveforms using PPG and ECG signals. Biomed Signal Process Control. 2023;79:104247. Available from: https://doi.org/10.1016/j.bspc.2022.104247
- Du J, Chang X, Ye C, Zeng Y, Yang S, Wu S, et al. Developing a hypertension visualization risk prediction system utilizing machine learning and health check-up data. Sci Rep. 2023;13:18953. Available from: https://www.nature.com/articles/s41598-023-46281-y
- Nematollahi MA, Jahangiri S, Asadollahi A, Salimi M, Dehghan A, Mashayekh M, et al. Body composition predicts hypertension using machine learning methods: a cohort study. Sci Rep. 2023;13(1):6885. Available from: https://www.nature.com/articles/s41598-023-34127-6
- D’Silva V, Desai G, D’Silva VA, Fernandes K, Cotta A, Cardoso S. Prediction of hypertension using machine learning. In: 2021 IEEE Bombay Section Signature Conference (IBSSC); 2021. p. 1-6. Available from: https://doi.org/10.1109/IBSSC53889.2021.9673470
- Wang ZC, Fan ZZ, Liu XY, Zhu MJ, Jiang SS, Tian S, et al. Deep learning for discrimination of hypertrophic cardiomyopathy and hypertensive heart disease on MRI native T1 maps. J Magn Reson Imaging. 2024;59(3):837-848. Available from: https://doi.org/10.1002/jmri.28904
- Montagna S, Pengo MF, Ferretti S, Borghi C, Ferri C, Grassi G, et al. Machine learning in hypertension detection: a study on World Hypertension Day data. J Med Syst. 2022;47(1):1. Available from: https://doi.org/10.1007/s10916-022-01900-5
- Dubey AK, Sinhal AK, Sharma R. Heart disease classification through crow intelligence optimization-based deep learning approach. Int J Inf Technol. 2024;16(3):1815-1830. Available from: https://doi.org/10.1007/s41870-023-01445-x
- Estiko RI, Rijanto E, Juwana YB, Juzar DA, Widyantoro B. Hypertension prediction models using machine learning with easy-to-collect risk factors: a systematic review. J Hypertens. 2024;42(Suppl 2):e19. Available from: https://doi.org/10.1097/01.hjh.0001027072.19895.81
- Wang R, Qi M, Shao Y, Zhou A, Ma H. Adversarial contrastive learning based physics-informed temporal networks for cuffless blood pressure estimation. arXiv. 2024. Available from: https://arxiv.org/html/2408.08488v1
- Tang Q, Tao C, Li X, Hu H, Chu X, Liu S, et al. Data-knowledge co-driven feature-based prediction model via photoplethysmography for evaluating blood pressure. Comput Biol Med. 2024;181:109076. Available from: https://doi.org/10.1016/j.compbiomed.2024.109076
- Turnip A, Taufik M, Kusumandari DE. Precision blood pressure prediction leveraging photoplethysmograph signals using support vector regression. Egypt Inform J. 2025;29:100599. Available from: https://doi.org/10.1016/j.eij.2024.100599
- Elahi A, Ali AA, Khan AH, Samad Z, Shahab H, Aziz N, et al. Challenges of managing hypertension in Pakistan: a review. Clin Hypertens. 2023;29(1):17. Available from: https://doi.org/10.1186/s40885-023-00245-6
- Ankışhan H, Celik H, Ulucanlar H, Yenigün BM. Early detection of high blood pressure from natural speech sounds with graph diffusion network. Comp Biol Med. 2025;185: 109591. Available from: https://doi.org/10.1016/j.compbiomed.2024.109591
- Hasanzadeh N, Valaee S, Salehinejad H. Hypertension detection from high-dimensional representation of photoplethysmogram signals. In: 2023 IEEE EMBS Int Conf Biomed Health Inform (BHI); 2023. p. 1-4. Available from: https://doi.org/10.48550/arXiv.2308.02425
- Islam SMS, Talukder A, Awal MA, Siddiqui MMU, Ahamad MM, Ahammed B, et al. Machine learning approaches for predicting hypertension and its associated factors using population-level data from three South Asian countries. Front Cardiovasc Med. 2022;9:839379. Available from: https://doi.org/10.3389/fcvm.2022.839379
- Baharoon M, Almatar H, Alduhayan R, Aldebasi T, Alahmadi B, Bokhari Y, et al. HyMNet: a multimodal deep learning system for hypertension classification using fundus photographs and cardiometabolic risk factors. arXiv [Preprint]. 2023. Available from: https://doi.org/10.3390/bioengineering11111080
- Duffy G, Cheng PP, Yuan N, He B, Kwan AC, Shun-Shin MJ, et al. High-throughput precision phenotyping of left ventricular hypertrophy with cardiovascular deep learning. JAMA Cardiol. 2022;7(4):386-395. Available from: https://doi.org/10.1001/jamacardio.2021.6059
- Evdochim L, Dobrescu D, Halichidis S, Dobrescu L, Stanciu S. Hypertension detection based on photoplethysmography signal morphology and machine learning techniques. Appl Sci. 2022;12(16):8380. Available from: https://www.mdpi.com/2076-3417/12/16/8380
- Mroz T, Griffin M, Cartabuke R, Laffin L, Russo-Alvarez G, Thomas G, et al. Predicting hypertension control using machine learning. PLoS One. 2024;19(3):e0299932. Available from: https://doi.org/10.1371/journal.pone.0299932
- Madhumitha S. Enhanced hypertension disease prediction using machine learning. 2024.
- Effati S, Kamarzardi-Torghabe A, Azizi-Froutaghe F, Atighi I, Ghiasi-Hafez S. Web application using machine learning to predict cardiovascular disease and hypertension in mine workers. Sci Rep. 2024;14(1): 31662. Available from: https://doi.org/10.1038/s41598-024-80919-9